Cardiovascular Medicine Center | Our Speciality
Our Speciality
We have been providing shifts in 24/7 coverage by attending physicians specializing in cardiovascular since the establishment of the chest pain center in July 2009. We cooperate with the emergency room to make an accurate diagnosis and utilize the latest coronary angiography and interventional equipment to restore blood flow in patients with acute myocardial infarction in order to decrease myocardial damage and improve prognosis. We achieve a rapid D2B time of 55 minutes which is far shorter than other medical centers do in Taiwan. Our center is now expanding the range of systematic care to accelerate the surgical preparation for heart failure and catheterization in patients with acute coronary syndromes.
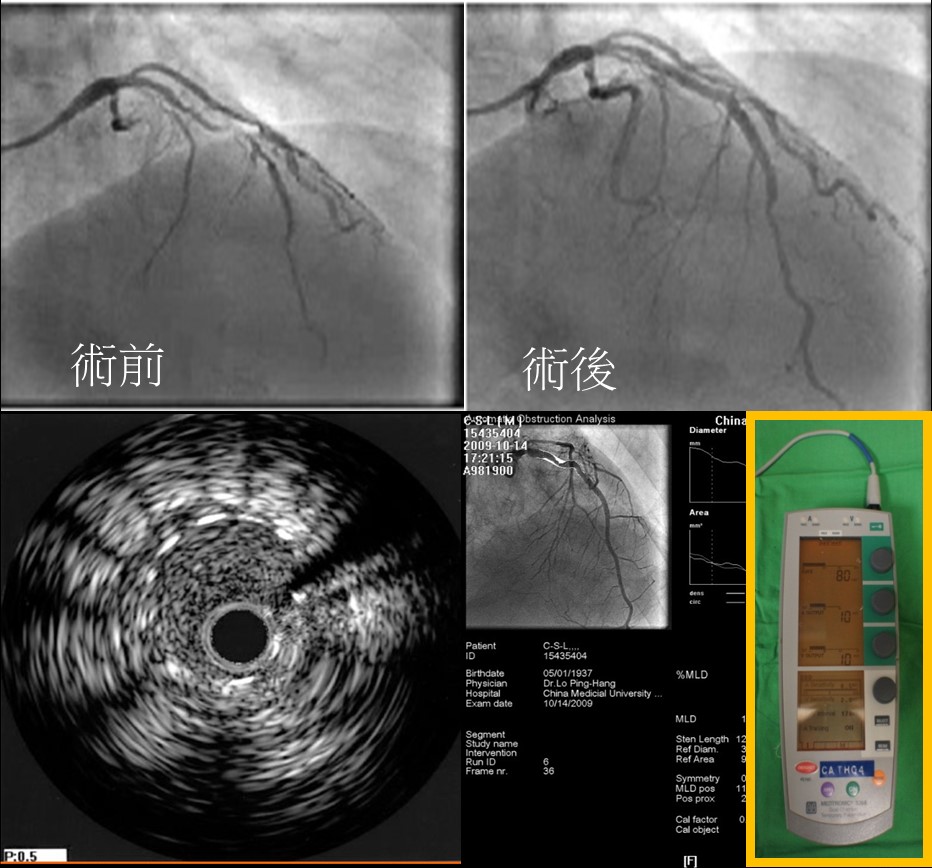
Our center has highly developed catheter interventional therapy. There are four cardiac catheterization rooms in which about 200 emergent cardiac catheterizations, 4000 cardiac catheterization, 700 coronary arterial drug-eluting stents placement and about 20 carotid artery stentings are performed every year. Every year since 2012, we have held national cardiac catheterization surgical demonstration and conference in February or March to display techniques for difficult cardiac catheterization which attracts interventional personnel come here sharing experiences. In 2016, the conference was expanded to international scale and demonstrated the surgical electrophysiology.

The mortality rate of calcific aortic stenosis is high in patients not treated surgically. In the past, the only way to treat calcific aortic stenosis was surgery, but many elderly patients could not bear the side effects of surgery. In recent years, TAVI has been developed and it has many advantages such as decreased invasion, lower risk, increased life expectancy and better life quality. In 2015, we established a hybrid operation room in which several TAVIs had been performed and the success rate is 100%.
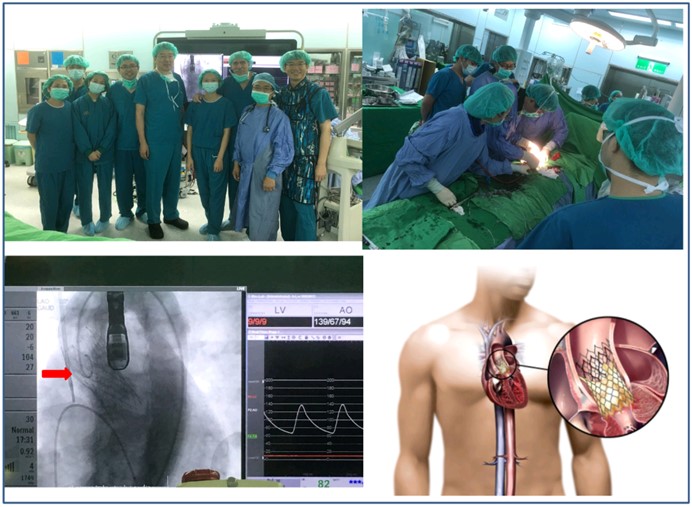
The risk of stroke is five times higher in patients with atrial fibrillation (AF) than in those without AF since that most thrombi in AF patients originate in the LAA. Preventive measures to avoid embolic events are permanent administration of anticoagulants, but several patients have got absolute or relative contraindication to this and thus are undertreated. To deal with this group of patients, left atrial appendage occlusion device placement has been developed. The device is guided through the catheter over the LAA in order to prevent blood clots from breaking off and thus lowers the risk of a stroke. We believe that this development will help lower patients’ risk of stroke and reduce the medical cost and the social cost. We have already performed 13 LAA occlude placements.
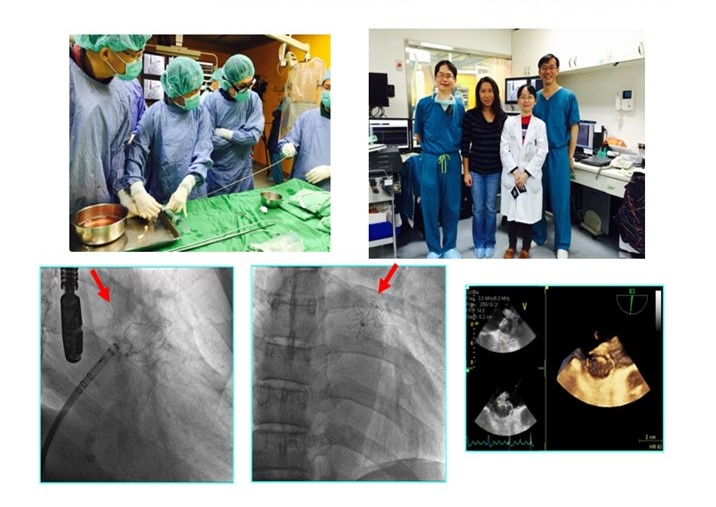
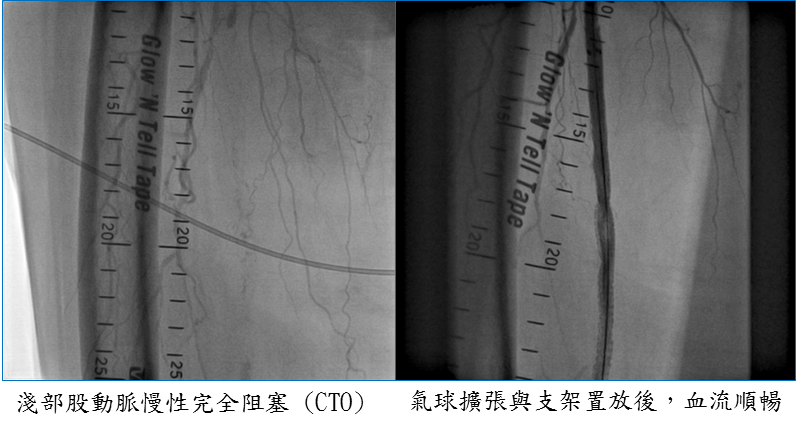
We are the only medical center in central Taiwan establishing a PVD care team which integrates the division of cardiovascular, cardiovascular surgery, endocrinology & metabolism, plastic surgery, orthopedics, infectious diseases, rehabilitation and hyperbaric oxygen therapy (HBOT) center. We established a thrombolytic emergency team which provides a timely thrombolytic therapy for patients with acute peripheral arterial occlusive disease (PAOD), acute pulmonary embolism and acute deep vein thrombosis (DVT). We are the most important medical center performing catheter assisted thrombolysis (EKOS) in Asia. We have performed about 150 cases of EKOS, of which the success rate in the lower extremity arteries is 100%, and the amputation rate is zero; the success rate in the pulmonary embolism is 100%; and the success rate in the DVT is 95%. We performed the world’s eighth lower limb deep vein arterialization in patients with PAOD failure to undergo bypass surgery or angioplasty, which is the first in East Asia. We have performed EKOS in eight patients with lower limb chronic DVT, of which the number is the most in Taiwan and the first in Asia. Furthermore, we actively developed the combined use of drug-eluting stents and laser in the therapy of lower limb. We became the world's pioneer and were invited to share our experience at the LEIPZIG interventional course (LINC).
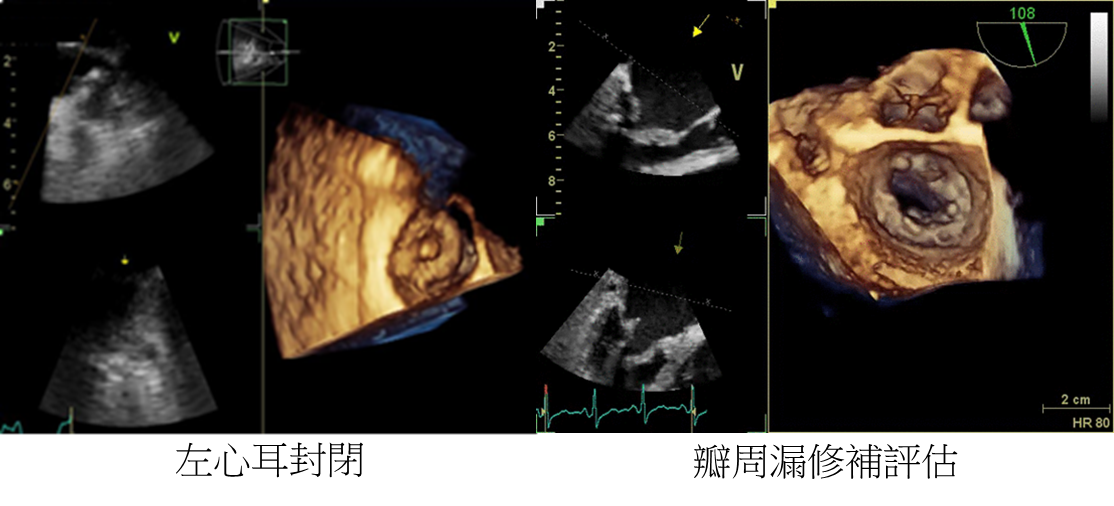
Since the improvement of cardiac catheterization, the therapeutic cardiac catheterization, replacing the traditional heart surgery, can be used in treatment of partial structural heart diseases such as atrial septal defect (ASD), ventricular septal defect (VSD) and LAA.
The x-ray in cardiac catheterization yields a 2D image; therefore, physicians will need TEE providing images at multiple angles. In recent years, there has been a breakthrough in the technique of ultrasound. TEE can offer real-time 3D images and provide excellent anatomic detail of the cardiac chambers and valves; thus, TEE decreases the difficulty of surgery and helps doctors guide the catheter more quickly.
The cooperation between advanced skills in TEE and interventional physicians provides different options for patients.
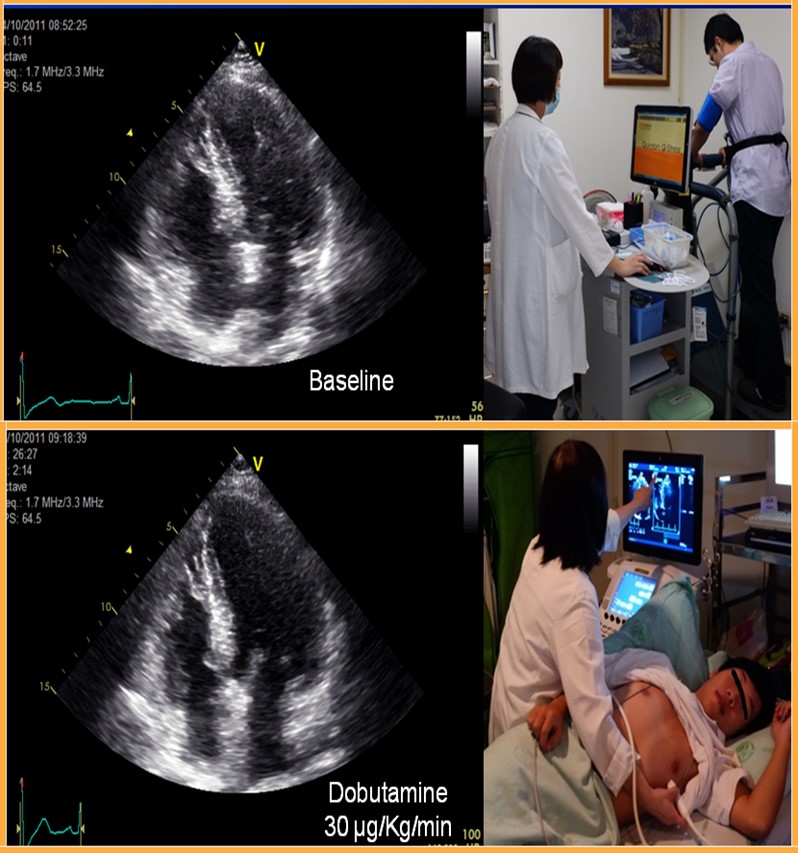
The echocardiography enables evaluation of cardiac function at rest while the stress echocardiography enables evaluation of cardiac function during exercise. Stress echocardiography can be accomplished using either exercise or cardiotonic agents.
Although a stress echocardiography requires a higher operator’s skill, it is still widely preferred in the West due to its lower risk, radiation-free nature and same accuracy as that of nuclear medicine.
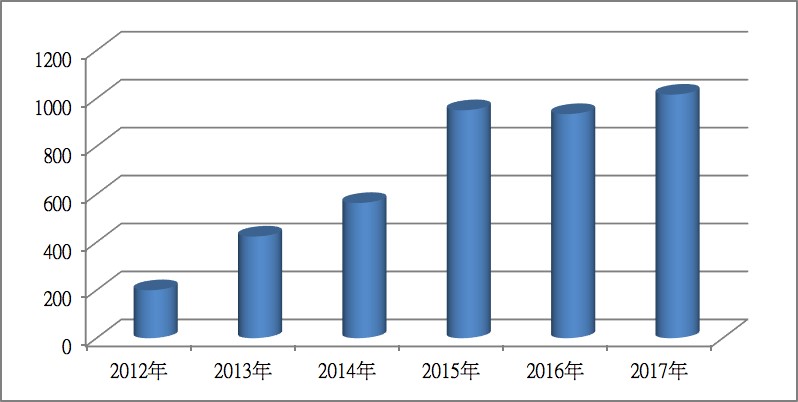
We have started performing a stress echocardiography since 2011. The number of cases increases every year. We perform almost 1000 cases of stress echocardiography every year, the most in Taiwan, and provide patients the most accurate examination.
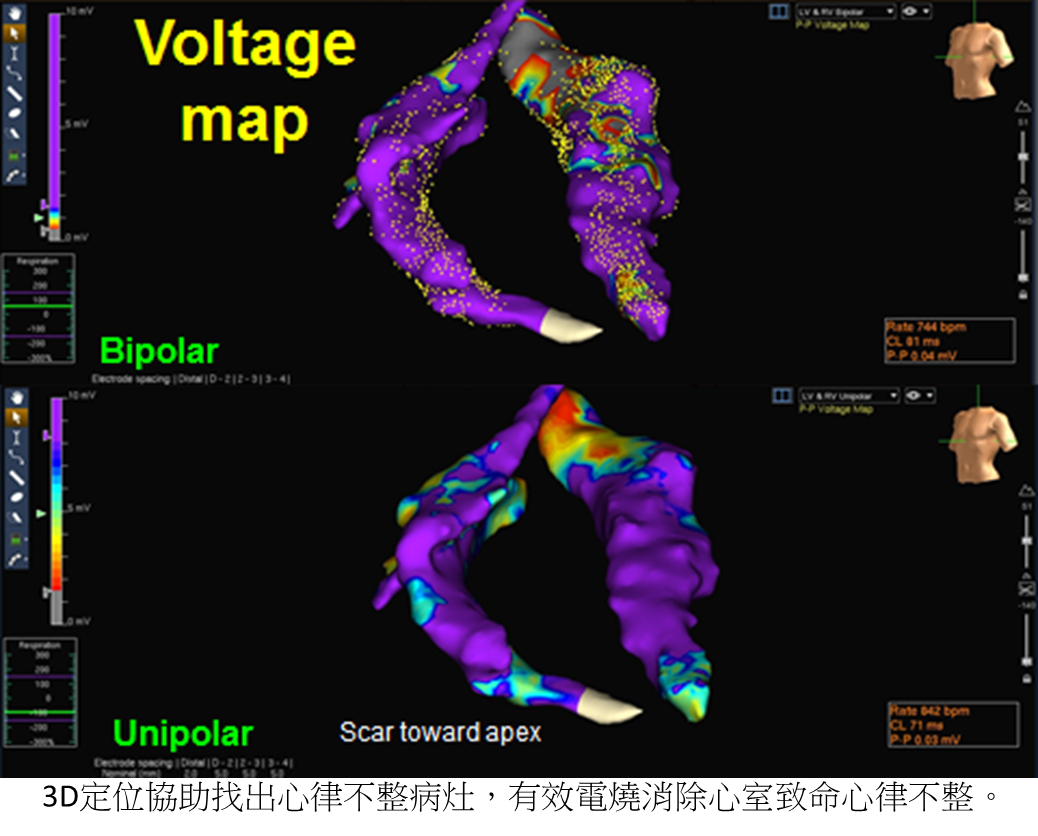
The system is composed of a miniature passive magnetic field sensor incorporated into a standard electrophysiological catheter and measures the electric field, the magnetic field or electromagnetic field of catheters in the heart; thus, the system generates an accurate 3D map. In addition, the system can also calculate the orientation the catheter tip, the signal strength and record the ablation process. Nowadays, the 3D mapping system can be accompanied by the cardiac CT or the magnetic resonance imaging to increase the accuracy and the resolution of image. The system also helps physicians realize the cause of arrhythmias and cardiac electrophysiology; thus, it increases the success rate of surgeries. Since traditional surgical ablation uses two-dimension x-ray imaging system, the success rate is low and the duration of operation is long in the ablation for complex arrhythmias such as atrial fibrillation, ventricular tachycardia, atypical atrial flutter and atrial tachycardia. However, since the 3D mapping system was developed, the success rate has been increased and the duration of operation has been shortened in the ablation for complex arrhythmias above. Since 2017, we have performed more than 270 cases of ablation for complex arrhythmias and the atrial fibrillation.
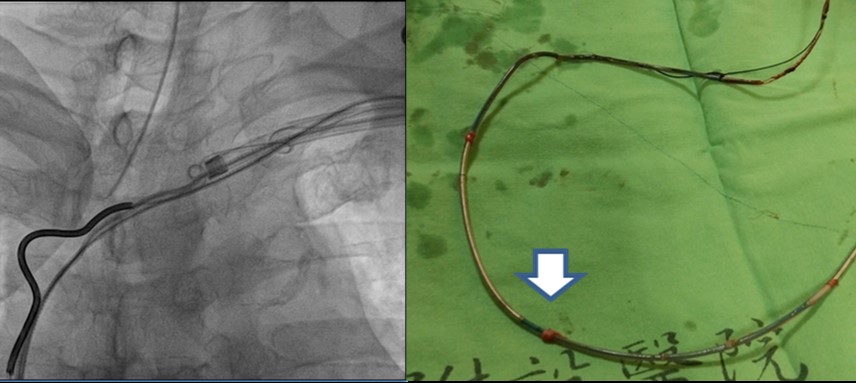
In cases of internal device infection, leads malfunction, excess leads, vessel blockage, or other clinical conditions, the patient implanted with a pacemaker or an implantable cardioverter defibrillator (ICD) need removing the battery and the set of threads. Removing the leads or wires installed over one year can be challenging because they may attach firmly with new connective tissues and blood vessels, a situation usually meets vessel laceration, severe hemorrhage, incomplete removal, or other complications if using conventional methods. To reduce complication and increase success rate of the procedure, the arrhythmia team of CMUH at the end of 2015 pioneered the laser-assisted extraction techniques across Taiwan to successfully remove the leads of a pacemaker and of an ICD; the procedure was performed in a part of central Taiwan. So far, the success rate of threads removal is 100% with 0% incidence of major complications.
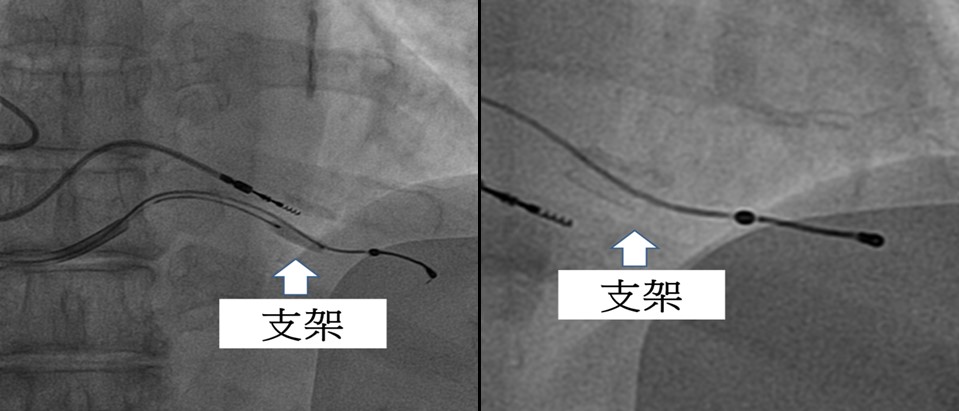
The arrhythmia team of CMUH also firstly used coronary stents to stabilize LV leads for the implantation of CRT. Placement of an LV CRT is known to be a critical treatment for patients with heart failure and left bundle-branch block. 60-70% of the treated patients can have improved cardiac function. The success rate of LV lead placement surgery is around 90%, but is variable depends on a patient’s coronary venomous anatomy: if no optimal placement location, deducted success rate is expected. Since June 2015 the team has performed the surgery in which coronary stents are placed at optimal locations to fix LV lead, thus increasing the success rate of CRT implantation. To date, 8 patients, whose LV leads were difficult to install, have received this procedure and have well-functioning leads.
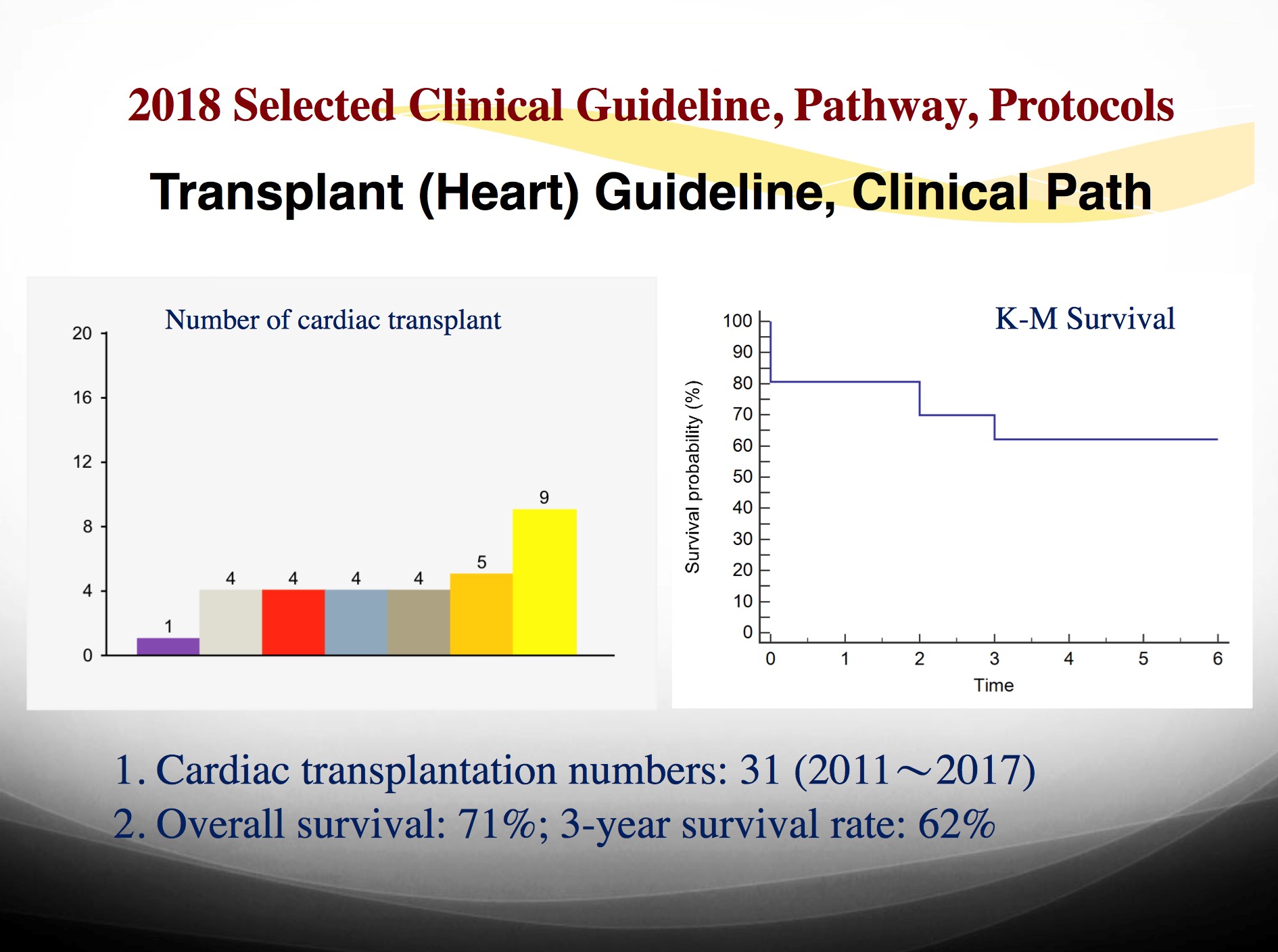
Some of those patients who have myocardial infarction or coronary condition, even having had their narrow vessels dredged, fail to regain fully recovered cardiomyocytes. This eventually results in severe heart failure that claims a mortality rate of 50% a year. Since 2011 the two divisions of cardiology and cardiovascular surgery have collaborated in heart transplantation. So far, 18 patients have received new hearts: a survival rate of 78%, an above-average standard nationwide. Among them 12 (86%) regain quality of life post-operatively and can live independently. Cardiovascular Center endeavors to develop heart transplantation techniques in hopes to offer life and hope to patients with heart failure.